Targeted Treatment Rooted in Understanding
Pain is not simply a symptom to be suppressed – it is a signal, a map, and in the right hands, a doorway to healing. At Somadelic Health, every procedure we offer begins with a fundamental question: what is your body asking for? With more than 40,000 interventional procedures performed across the full spectrum of spinal and joint conditions, we bring an uncommon depth of experience to that question – and an equally uncommon precision in answering it.
Each procedure described here is guided by advanced imaging, individualized diagnostic data, and a care philosophy rooted in working with the body rather than around it. Whether you are navigating disc pain, facet arthritis, nerve compression, or a condition that has not yet been properly named, we invite you to explore what targeted, evidence-based intervention can offer.
Transforming Brain Health, Restoring Balance
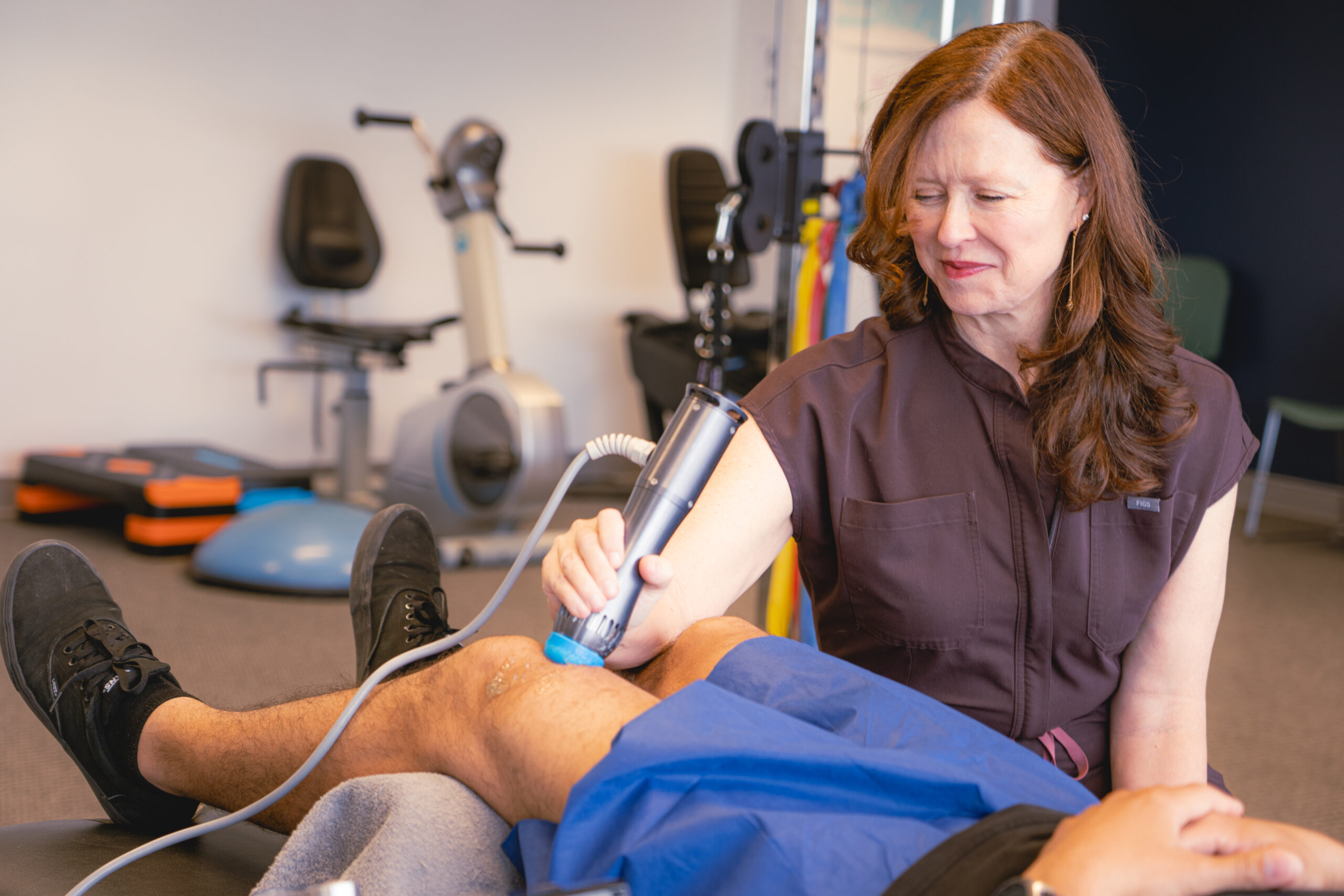
Our Approach to Healing
You’ll receive a thorough evaluation, a clear explanation of your brain health, and a step-by-step plan for care. Our team supports you at every stage, helping you reclaim clarity, calm, and control.

Precision Diagnostics
We use advanced neuro-assessment tools to map your brain’s unique patterns and identify underlying imbalances.

Personalized Plans
Your treatment is tailored to your specific symptoms, history, and goals, ensuring the most effective path to recovery.

Integrative Support
We combine neuroplasticity-based therapies, medication management, and lifestyle guidance for comprehensive healing.
Unlock your body’s natural healing potential with personalized treatments.
Each procedure at Somadelic Health is carefully designed to identify and treat the underlying source of your pain. Guided by advanced imaging and individualized diagnostics, our approach targets spinal and joint conditions with precision—supporting natural healing, restoring function, and delivering lasting relief through evidence-based, patient-centered care.
Foundational Spinal & Joint Procedures
Epidural Injection: Treating the Nerves of the Spine
The nerves that carry sensation and movement throughout your body travel through the spine in a protective canal surrounded by a layer of tissue called the epidural space. When those nerves become inflamed – from a herniated disc pressing against them, from spinal narrowing, or from the chemical irritants that an injured disc can release – the pain can be profound and far-reaching, radiating down the arm or leg, disrupting sleep, and limiting everyday life.
Facet Joint Injection: Treating the Joints of the Spine
Your spine is not simply a column of bones – it is a series of paired joints called facet joints (also known as zygapophysial joints), one on each side at every spinal level. These small but critical joints guide and constrain your spine’s movement, and like any joint in the body, they can develop arthritis, become inflamed after an injury, or simply wear over time. When they do, they produce a characteristic deep, aching pain – often worse in the morning, aggravated by twisting or extending the spine, and sometimes referring into the shoulders, buttocks, or thighs in patterns that can be easily mistaken for disc or nerve pain.
Discography: Evaluating the Discs of the Spine
The intervertebral discs – those resilient, shock-absorbing structures that sit between each pair of vertebrae – are among the most common yet most difficult sources of spinal pain to diagnose. Standard imaging such as MRI can show structural changes in a disc, but it cannot always tell us whether that disc is the source of your pain. Two patients can have similar-appearing disc abnormalities on imaging, yet have entirely different pain experiences.
Sacroiliac Joint Injection: Treating the Joints of the Pelvis
The sacroiliac (SI) joints connect your spine to your pelvis, one on each side, and they bear the full load of your upper body with every step you take. Despite their central role in movement and weight-bearing, the SI joints are frequently overlooked as a source of low back and pelvic pain – studies suggest they contribute to pain in up to 30% of patients with chronic low back complaints, yet they are often dismissed or misattributed.
Hip Joint Injection
Hip pain is common, but it is not simple. The hip is a deep ball-and-socket joint capable of generating pain locally – in the groin, lateral hip, or buttock – or referring to the lower back, thigh, or even the knee in patterns that confuse both patients and clinicians. Arthritis, labral tears, bursitis, and tendinopathy can all produce overlapping symptoms, and the distinction between intra-articular (inside the joint) and extra-articular pain sources matters enormously for treatment.
Shoulder Joint Injection
The shoulder is the most mobile joint in the human body – and that mobility comes at the cost of inherent vulnerability. Rotator cuff pathology, glenohumeral arthritis, adhesive capsulitis, and bicipital tendinopathy are among the most common pain generators we treat, often in patients who have been managing discomfort for months before seeking targeted care.
Cervical (Neck) Procedures
The cervical spine is one of the most complex – and most consequential – regions we treat. Seven vertebrae, eight nerve roots, and a network of joints responsible for the full range of head movement all converge in a remarkably compact space. Cervical pain is rarely simple: it may arise from joints, discs, nerves, or any combination, and it frequently refers to the head, shoulders, and arms in patterns that require careful diagnostic thinking. Our approach to the cervical spine reflects its complexity – methodical, precise, and always guided by imaging.
Lateral Atlanto-Axial Joint (C1-C2) Access
The atlanto-axial joint – the joint between the first and second cervical vertebrae – is responsible for approximately half of your head’s rotation. When this joint becomes arthritic or inflamed, it produces a characteristic deep, aching pain at the top of the neck, often accompanied by headaches that radiate to the back of the skull and sometimes into the ear or eye.
Cervical Zygapophysial (Facet) Joint Procedures
The cervical facet joints are among the most common sources of neck pain and cervicogenic headache, yet they are underrecognized in standard clinical evaluations. Pain from these joints can present as neck stiffness, focal tenderness, and headaches that originate at the base of the skull and radiate forward – a pattern sometimes mistaken for tension or migraine headache.
Cervical Medial Branch Blocks
The medial branch nerves are the small sensory nerves that carry pain signals from the cervical facet joints to the brain. Blocking these nerves with local anesthetic – under fluoroscopic guidance – is the most precise way to confirm a facet joint as a source of pain. Two sets of medial branch blocks, performed on separate occasions, are considered the gold standard diagnostic test before any decision about radiofrequency neurotomy.
Third Occipital Nerve Blocks
The third occipital nerve is a branch of the third cervical dorsal ramus and is the primary innervation of the C2-C3 facet joint. This nerve is one of the most frequently overlooked sources of cervicogenic headache – headaches that originate in the upper cervical spine and refer to the occiput, behind the eye, and into the temple.
Cervical Medial Branch Thermal Radiofrequency Neurotomy
When diagnostic medial branch blocks confirm that cervical facet joints are a significant source of your pain, radiofrequency neurotomy offers the possibility of longer-lasting relief. This procedure uses precisely controlled thermal energy to interrupt the pain-transmitting nerves – without affecting the motor nerves that control muscle function.
Cervical Interlaminar Epidural Access
Cervical epidural procedures allow us to deliver medication directly to the epidural space of the neck, bathing the spinal cord and nerve roots in anti-inflammatory agents and providing relief for conditions ranging from herniated cervical discs to post-surgical scar tissue and spinal stenosis.
Cervical Disc Stimulation (Provocation Discography)
Cervical discogenic pain – pain arising from within the disc itself rather than from nerve compression – is one of the most challenging diagnoses in spine care. The disc contains pain-sensitive nerve fibers in its outer layers, and disruption of these fibers through internal tears or degeneration can cause deep, aching anterior neck pain, often with headache and referral into the shoulder and interscapular region.
An Algorithm for Cervical Synovial Joint Assessment
At Somadelic Health, we do not perform procedures in isolation. For patients with cervical pain of uncertain origin, we follow a systematic diagnostic algorithm: a thorough clinical history and physical examination, review of imaging, targeted diagnostic blocks in a logical sequence, and data-driven decisions about treatment.
Thoracic (Mid-Back) Procedures
The thoracic spine is the least commonly treated region of the spine – but it is by no means immune to pain. Thoracic facet arthritis, disc disease, and nerve root irritation are frequently underdiagnosed, particularly in patients who have had thoracic pain attributed to muscular causes for years. We bring the same diagnostic rigor to the thoracic spine that we apply to the cervical and lumbar regions.
Thoracic Transforaminal Access
Applications of Thoracic Transforaminal Access
Thoracic transforaminal injections deliver medication directly to the thoracic nerve roots – the nerves that wrap around the chest wall and can produce intercostal neuralgia, post-herpetic neuralgia (shingles-related nerve pain), and thoracic radiculopathy. For patients with these conditions, transforaminal access can be both diagnostically illuminating and therapeutically meaningful.
Thoracic Zygapophysial (Facet) Joint Procedures
Applications of Thoracic Zygapophysial Joint Access
The thoracic facet joints can be a significant source of mid-back pain, particularly in patients with thoracic scoliosis, Scheuermann’s kyphosis, or post-traumatic degeneration. Intra-articular injections and medial branch blocks of the thoracic facet joints follow the same diagnostic and therapeutic logic as their cervical and lumbar counterparts – confirming the joint as a pain source and providing targeted relief.
Thoracic Medial Branch Blocks
Thoracic medial branch blocks are the diagnostic precursor to thoracic radiofrequency neurotomy for facet-mediated mid-back pain. Performed under fluoroscopic guidance, these blocks involve placing local anesthetic precisely onto the medial branch nerves at the relevant thoracic levels, and monitoring your response to determine whether the facet joints are contributing to your pain.
Lumbar (Lower Back) Procedures
Low back pain is one of the most prevalent conditions in human health, and yet it is also one of the most imprecisely treated. The majority of patients with chronic low back pain have never had a specific structural diagnosis confirmed by diagnostic blocks – they have had imaging findings and educated guesses. At Somadelic Health, we change that equation. Every lumbar procedure we perform is grounded in systematic diagnostic thinking, and every treatment decision follows from evidence, not assumption.
Lumbar Zygapophysial (Facet) Joint Access
Applications of Lumbar Zygapophysial Joint Access
The lumbar facet joints are among the most common identifiable sources of chronic low back pain, contributing to symptoms in approximately 15-45% of patients with non-specific low back pain. Facet-mediated pain typically presents as axial lower back pain that is worse with extension and rotation, and that may refer into the buttocks and upper thighs without the sharp, shooting quality of nerve root pain.
Lumbar Intervertebral Disc Access
The lumbar discs are the most common structural abnormalities found on spinal imaging – but finding a degenerated or herniated disc on MRI does not automatically identify it as the source of pain. Our approach to lumbar disc disease is guided by this fundamental distinction, and we use diagnostic discography when the clinical question genuinely requires it.
Lumbar Transforaminal Access
Lumbar and Sacral Spinal Nerve Blocks
Lumbar and sacral spinal nerve blocks place local anesthetic directly alongside a specific nerve root as it exits the spinal canal, allowing us to confirm that nerve’s contribution to your symptoms. When sciatica or radicular pain is present, nerve block responses help us identify the precise level responsible – information that is critical when multiple levels appear abnormal on imaging.
Lumbar Interlaminar Epidural Access
Lumbar Epidural Steroids
Lumbar interlaminar epidural steroid injections access the epidural space from the back of the spine, distributing anti-inflammatory medication broadly across the spinal canal. This approach is appropriate for bilateral radicular symptoms, spinal stenosis, and conditions where the nerve root level is less precisely localized. Performed under fluoroscopic guidance with contrast confirmation, interlaminar epidurals are among the most commonly performed and most thoroughly studied interventional spine procedures.
Lumbar Medial Branch Blocks
Lumbar medial branch blocks are the definitive diagnostic test for lumbar facet joint pain. Two sets of comparative medial branch blocks – each using a different local anesthetic – are required to confirm the diagnosis with sufficient confidence before radiofrequency neurotomy is considered. This rigorous standard exists because the research literature is unequivocal: the more carefully the diagnosis is established, the better the outcome of the treatment.
Lumbar Medial Branch Thermal Radiofrequency Neurotomy
Lumbar radiofrequency neurotomy is one of the most effective evidence-based treatments available for chronic facet-mediated low back pain. By using carefully controlled thermal energy to interrupt the pain-transmitting medial branch nerves, we can provide relief that lasts months to years – far longer than injections alone.
An Algorithm for the Investigation of Low Back Pain
Low back pain has more potential sources than any other pain condition – discs, facet joints, sacroiliac joints, nerve roots, muscles, and combinations of all of them. At Somadelic Health, we approach low back pain not as a single diagnosis but as a diagnostic investigation. Our algorithmic framework – derived from international evidence-based guidelines and refined by more than 40,000 procedural encounters – ensures that we follow the most clinically rational pathway to your specific diagnosis.
Sacral Procedures
The sacrum and sacroiliac joints represent the critical interface between the spine and the pelvis – a transition zone that bears enormous mechanical loads and that is, in many patients, an unrecognized source of chronic pain. Our sacral procedures bring the same diagnostic precision and evidence-based approach that characterizes all of our work.
Sacroiliac Joint Blocks
Sacroiliac joint blocks are the diagnostic reference standard for confirming SI joint-mediated pain. Under fluoroscopic or CT guidance, local anesthetic is placed within the joint and its posterior ligamentous complex – both of which are pain-generating structures – and your response is carefully monitored. A positive response to a sacroiliac block is the basis for all subsequent targeted treatment decisions.
Sacroiliac Intra-Articular Injection of Steroids
When the sacroiliac joint is confirmed as a pain source, intra-articular corticosteroid injection delivers potent anti-inflammatory medication directly into the joint, reducing the inflammatory activity that drives pain and disability. For many patients, SI joint injections provide months of meaningful relief. For those seeking longer-term options, we also discuss regenerative treatments – including platelet-rich plasma delivered directly to the posterior SI ligamentous complex – which has shown promising results for sustained pain reduction in this challenging anatomical region.
Your pain has a source. We intend to find it.
Every procedure described here is a tool – and like all tools, it is only as good as the judgment and precision with which it is used. At Somadelic Health, we bring more than four decades of combined procedural experience, advanced imaging guidance, and a commitment to diagnostic accuracy that we believe is rare. We also bring something that does not appear in clinical trials: the willingness to sit with you, understand your specific situation, and build a plan that reflects who you are – not just what your MRI shows.
If you would like to explore whether any of these procedures are appropriate for your pain, we invite you to schedule a consultation. Come with your questions, your imaging, and your history. We will bring everything else.
